Highlight
Increasing Efficacy for Lung Cancer Chemotherapeutics: Targeted Drug Delivery via the Protocell
Achievement/Results
According to current statistics reported by the Center for Disease Control and Prevention (CDC) lung cancer is the second most common cancer in both men and women. Lung cancer is also behind a third of all cancer related deaths in the United States. Astonishingly more people die of lung cancer than of colon, breast, and prostate cancers combined. There is a definite necessity for advancement in the area of lung cancer research. Lung cancer is divided into two different types including small cell and non-small cell. Since Non-Small Cell Lung Cancer (NSCLC) accounts for 85-90% of all lung cancer cases, this research is focused on NSCLC. The typical survival for patients with advanced stage NSCLC is 6 months for untreated patients and only a mere 3 months more for patients treated with chemotherapy. The reported 5-year survival rate of patients with advanced NSCLC is less than 10%.
These statistics strongly indicate a need to break through the ceiling of low clinical efficacy in lung cancer chemotherapeutics. Thus, increasing the clinical efficacy of lung cancer chemotherapeutics is an area of high interest, which will foster research that will have far reaching implications for increasing the quality of life for people suffering from lung cancer. The therapeutic efficacy of ‘free’ drugs is often hindered by non-specific toxicity that arises from the cytotoxic effects of the drug(s) on healthy cells. In efforts to improve therapeutic efficacy of cancer therapies formulation methods of drug encapsulation or complexation with liposomes, polymers, or proteins have been employed. However, while treatments using such strategies are clinically available they rely on passive target principles such as the drug permeability and retention effect. Currently there are few clinically-approved treatments that selectively target diseased cells via specific biomolecular interactions.
Research project of Annikka Jensen, an INCBN IGERT Trainee, involves targeted drug delivery to cancer cells via engineered mesoporous nanoparticle-supported lipid bilayers (protocells), a new class of targeted nanocarriers. This new class of targeted nanocarriers holds significant promise for improving the efficacy of cancer treatments as their combination of specificity, stability, and enhanced cargo capacity, allows for the capability of delivering a high concentration of the drug directly to the human cancer cell with minimal systemic toxicity. Initial in vitro experiments have demonstrated that SP94 conjugated protocells are able to specifically target and kill human hepatocellular carcinoma (HCC) cells with orders of magnitude greater efficiency than ‘free’ or liposomal encapsulated drug, even in multiple drug resistant variants. Extending this research to in vitro NSCLC models will assist in leading to significant increases in the efficacy of current lung cancer chemotherapeutics by reducing the growth of human lung adenocarcinoma/carcinoma cells, including multiple drug resistant variants, greater than the corresponding ‘free’ or liposomal-delivered drug by harnessing the combined power of the protocell targeted drug delivery system and localized direct delivery of the chemotherapeutics via the inhalation route to the lungs.
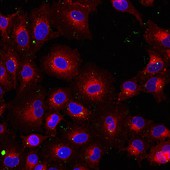
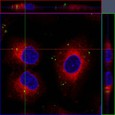
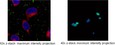
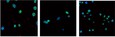
This discovery work will facilitate establishing the nation as a global leader in transforming the field of targeted drug delivery. For initial studies, confocal fluorescence microscopy experiments have been performed with the positive control, A549 cell line, and the negative control, BEAS-2B cell line to establish that the NSCLC cell lines will be able to have preferential delivery of the based on the use of a targeting peptide. For these initial experiments, a well established EGF peptide, with sequence YHWYGYTPQNVI, was chosen as a targeting peptide, since it binds to the well established overexpressed EGFR receptor in NSCLC cell lines. The EGF peptide was at saturating levels on the and the delivered concentration of the protocells was at saturating levels. The results of these initial binding studies show that NSCLC cells can be selectively targeted using protocells modified with EGF peptide. Virtually no non-specific targeting to non-cancerous cells is observed.
Address Goals
Primary Goal: Protocells have demonstrated remarkable cell targeting specificity and cancer cytotoxicity with hepatocarcinoma in vitro studies and show promise in serving as a universal targeted drug delivery system; however, their efficacy with non-small cell lung cancer in vitro remains unknown. Results from this project will cultivate world-class knowledge regarding the toxicity and therapeutic efficacy of this engineered nanoparticle drug delivery system in vitro, facilitating development of protocells for in vivo inhalation studies.
Secondary Goal: In vivo inhalation biodistribution, toxicity, and pharmacokinetic studies will build the nation’s research capability by supporting the translation of protocells from the lab bench to the clinic to serve as a direct targeted drug delivery system for non-small cell lung cancer treatment.